Welcome back. Today’s post is a big one. As the title suggests, this will be a deep dive into the specifics of my transplant.
The goal of this post is to provide a more detailed account of what my experience consisted of in terms of my type of transplant, donor details, medications, chemotherapy agents, side effects, and more.
Because of that, this post, more than just about any other I have shared to date, will only really be applicable to those who want to get a concrete idea of what receiving a transplant can actually look like in full detail.
It will be very information-heavy, with plenty of outside sources referenced.
Before I get started though, I want to state something very clearly. None of what I discuss today should be taken as medical advice. I try to include a disclaimer like this in every post, but it is especially important given the topics we will be covering today.
Every transplant experience is different. There may be some overlap, and that is part of why I moved forward with writing this, but your experience will likely be unique in more ways than one.
Please do not let the information I share here replace the experience, education, qualifications, and advice of your actual care team.
With that extended disclaimer out of the way, let’s get started. I will be breaking this post down into sections, moving from pre-transplant through to the present day. Any additional medications or treatment I end up needing will be discussed in the periodic Field Note updates that I share.
Pre-Transplant
One of the more apparent ways my experience differs from many others is the timing of my diagnosis. We found out about my genetic mutation at what was probably the most optimal time possible. Early enough to plan and act effectively, but far enough along for my care team to initially recognize that something was not right.
Because of that, this will be the shortest section of the bunch. In the eight-month period between my diagnosis and deciding to proceed with the transplant, we simply monitored and made decisions based on the results from the countless tests I underwent.
All of which are discussed in detail in my Pre-Transplant Testing post.
I did not require any prior conditioning or treatment of any kind. No radiation or anything like that. We went straight to transplant. Zero to a hundred.
That said, there are two medications that belong in this section. One was given to me before the two bone marrow biopsies I had prior to transplant, and the other I started approximately two weeks before being admitted.
- Lorazepam (Ativan) – Ativan is “used for short-term relief of the symptoms of anxiety or anxiety caused by depression.” It is my understanding that use of Ativan, or some other anti-anxiety medication, is relatively common prior to undergoing the biopsy procedure.
- My Dosage: 0.5mg. Oral medication. 15 minutes prior to initiating the biopsy procedure.
- Ursodiol (Actigall) – Actigall is usually given to dissolve gallstones in your liver and prevent any bile duct buildups. In the transplant setting, Actigall works as a prophylactic, with the goal of preventing any liver issues as treatment begins. More proactive than anything else. Veno-occlusive disease (VOD)/ Sinusoidal obstruction syndrome (SOS) being the main things Actigall attempts to prevent.
- My Dosage: 300mg. Oral medication. Three times a day. Began approximately two weeks before admission to “prep” my liver for the strain of treatment.
As far as pre-transplant medications go, that is it for me. I acknowledge how lucky I am in that respect.
But like everyone who undergoes a transplant, the days in the hospital are much more intense and involve a lot more medications and treatment, all of which we are about to get into.
The caveat with discussing all that is that with a medication and treatment list as long as one has while moving through transplant, describing how each individual thing made me feel is simply impossible.
It’s a cocktail to say the least, so while I’ll be listing and defining all of the individual meds and treatment I received, I will only be directly discussing a few of the medications/drugs that stood out or that are directly mentioned in my medical records as being slightly problematic.
Transplant Conditioning (Days -6 – -1)
I don’t think there is a better place to start than with the chemotherapy agents used for my transplant, as many of the other medications discussed, especially early on, are meant to help your body cope with the effects of the chemo.
Chemotherapy Agents
- Busulfan (Busulfex) – Busulfan belongs to a group of medicines known as alkylating agents. These agents are very common in cancer treatment. Busulfan has existed for a while in oral form, but developments in the IV version of administering it has made it a much more viable choice for a lot of transplant centers. I only know that by reading a few paragraphs of “Busulfan in Hematopoietic Stem Cell Transplantation,” which I’d recommend checking out if you want a more detailed account of the history of the drug and why it is being used more commonly in the transplant setting.
- My Dosage: 59mg in sodium chloride 0.9% 118mL. IV infusion. 16 doses total. Administered every 6 hours. Each dose took roughly 3 hours. First dose on day -5. Last dose on day -1.
- Fludarabine (Fludara) – Fludarabine was the counterpart of choice to Busulfan in my scenario. The main purpose of Fludarabine is to inhibit the growth of new cancer cells while I received treatment. This combination (busulfan + fludarabine) is one of the more studied chemo combinations for myeloablative transplant patients, specifically those with certain types of Leukemia.
- My Dosage: 54.25mg in sodium chloride 0.9% 112.17 mL. IV infusion. 4 doses total. Administered every 24 hours. Each dose took roughly 30 minutes. First dose on day -5. Last dose on day -2.
The goal of every transplant conditioning regimen, in almost every case, is to eliminate or suppress your existing marrow and immune system enough to make space for the donor cells to engraft as smoothly as possible.
That, of course, is much easier said than done. The agents and dosages your team chooses will take into account your underlying disease and its behavior, your disease status at the time of transplant, your age and overall health, your organ function, your donor type, quality of the match, risk of relapse versus risk of toxicity, institutional protocol/physician experience, emerging research, etc.
My recommendation, as always, is to listen to your care team and do your own research on the specific regimen that is chosen for you based on all the factors listed above.
In my case, we opted for what is known as a myeloablative regimen. Essentially, the “scorched earth” option as far as pre-transplant conditioning goes. While intimidating, it was the option that my team felt most confident moving forward with and the one that would provide me with the best shot at truly ridding my marrow of the mutation I have.
All the different types of transplants, conditioning practices, and ways in which you can actually receive a transplant can be found here, courtesy of Dana-Farber.
Additional Medications
In conjunction with starting the conditioning, I was also given a wide range of medications meant to support my body in different ways and to ultimately prepare me for receiving the transplant.
- Acyclovir (Zovirax) – Traditionally used to treat shingles, herpes (HSV), and chickenpox. Used in the transplant setting as an anti-viral/prophylaxis to prevent these from occurring or resurfacing while your new immune system re-builds.
- My Dosage: 400mg. Oral medication. Three times a day. First dose on day -5. Have taken daily since.
- Bisacodyl (Dulcolax) – A mild stimulant laxative, meant to increase the stimulus in your intestines to encourage a bowel movement.
- My Dosage: 5mg. Oral medication. Once a day. Took on day -2. As needed for moderate constipation.
- My Dosage: 10mg. Oral medication. Once a day. Took on day 0. As needed for moderate constipation.
- Chlorhexidine (Peridex) – Used to reduce inflammation and bacteria presence in your mouth. Commonly used to treat gingivitis.
- My Dosage: 0.12% 5mL. Oral rinse. Twice a day. First dose on day -2. Last dose on day +17.
- Chlorhexidine Gluconate – Same drug more or less as listed above, but in wipe form. Used in the hospital/transplant setting to kill bacteria on the skin.
- My Dosage: 2%. Topical wipe. Once a day. First introduced on day -6. Used through day +17.
- Cholecalciferol (Vitamin D3) – Dietary supplement used to treat vitamin D deficiency. In addition to supporting your bone health, having a healthy vitamin D level actually supports your immune system as well, which is crucial in the early stages of recovery.
- My Dosage: 25mcg. Oral medication. Once a day. First dose on day -1. Have taken daily since.
- D-5-½ NS with KCL 20 mEq/L – While I think the name could use some workshopping, this is less daunting than it sounds. Essentially, it’s dextrose 5% in 0.45% sodium chloride with potassium chloride. Fancy words for electrolytes and fluids. That’s all.
- My Dosage: 100 mL/hr. IV infusion. Continuous. First dose on day -5 along with initial Busulfan dose. Continued until I was 24 hours removed from last dose of chemo.
- Enoxaparin (Lovenox) – Used to prevent deep venous thrombosis (DVT), a condition in which harmful blood clots form in the blood vessels in your legs. The chemo will be knocking your counts all the way down, so this helps prevent any clots and reduce the risk of excess bleeding from occurring due to low platelet counts.
- My Dosage: 40mg. Subcutaneous injection (typically stomach or leg). Once a day. 5 doses total. First dose on day -5. Last dose on day -1.
- Folic Acid (Folvite) – Supports your body’s ability to produce healthy and functional red blood cells.
- My Dosage: 1mg. Oral medication. Once a day. First dose on day -5. Have taken daily since.
- Lactulose (Constulose) – Promotes bowel movements.
- My Dosage: 20g. Powdered solution. Once a day. Took on day -1.
- Levetiracetam (Keppra) – Given to reduce the risk of certain types of seizures from occurring while receiving Busulfan. It essentially calms your neurotransmitters down and prevents any excessive activity from setting off a seizure.
- My Dosage: 500mg. Oral medication. Every 12 hours. First dose on day -5 alongside initial Busulfan dose. 14 doses total. Last dose on day +1.
- Lorazepam (Ativan) – In addition to calming anxiety, Ativan has also been known to reduce feelings of nausea. Both of which are present most of the time while undergoing a transplant.
- My Dosage: 0.5mg. Oral medication. Every 6 hours. First dose on day -5. As needed. Last dose on day +6.
- Magnesium Sulfate – Helps maintain the balance of electrolytes in the body, preventing any complications from having low levels.
- My Dosage: 2g/50 mL (4%). IV infusion. Administered as needed. First dose on day -5.
- My Dosage: 4g/100mL (4%). IV infusion. Administered as needed. First dose on day -1.
- Multivitamin (MVI) – Provides your body with nutrients you may or may not be receiving enough of through your diet.
- My Dosage: 1 pill. Oral medication. Once a day. First dose on day -5. Have taken daily since.
- Neomycin (Neo-Fradin) – An antibiotic that is meant to prevent bacterial infections in the intestines.
- My Dosage: 500,000 units. Oral rinse. Three times a day. First dose on day -1. Last dose on day +17.
- Olanzapine (Zyprexa Zydis) – Typically used to help treat patients with schizophrenia or bipolar disorder. In the transplant setting, it can be used to block certain neurotransmitters that are associated with causing nausea and vomiting.
- My Dosage: 5mg. Oral medication. 2 times a day. First dose on day -2. Last dose on day +16.
- Ondansetron (Zofran) – Used to prevent, or at least lessen, chemotherapy induced nausea and vomiting.
- My Dosage: 8mg. IV injection. Every 8 hours. 15 doses total. First dose on day -5. Last dose on day -1.
- Palonosetron (Aloxi) – Similar to Zofran, Aloxi is used to lessen the frequency and severity of chemotherapy induced nausea and vomiting.
- My Dosage: 0.25mg. IV injection. Once every 3 days. First dose on day -2. Last dose on day +14.
- Polyethylene Glycol – A laxative solution that aims to increase the amount of water moving through your intestinal tract.
- My Dosage: 17g. Powdered solution. Once daily as needed. Took on day -3 and again on day +1.
- Polymyxin B – Used to treat bacterial infections. Serves as a prophylactic in the transplant setting.
- My Dosage: 1m units. Oral medication. Every 8 hours. First dose on day -1. Last dose on day +16.
- Prochlorperazine (Compazine) – Traditionally used to treat certain mental conditions, but used in the transplant setting to temper severe nausea and vomiting.
- My Dosage: 10mg. Oral medication. Every 6 hours as needed. First dose on day -2. Last dose on day +8.
- My Dosage: 10mg. IV Injection (faster acting). Every 6 hours as needed. First dose on day -2. Last dose on day +11.
- My Dosage: 2 tablets. Oral medication. Two times per day as needed. Taken on day 0 and day +1.
- Sulfamethoxazole-Trimethoprim (Bactrim) – An antibiotic used to eliminate certain bacteria that can be very problematic for those with weakened immune systems.
- My Dosage: 160mg. Oral medication. Every 12 hours. 11 doses total. First dose on day -6. Last dose on day -1.
- Ursodiol (Actigall) – Same as in the pre-transplant buildup, Actigall works as a prophylactic, with the goal of preventing any liver issues as treatment begins.
- My Dosage: 300mg. Oral medication. Three times a day. Began approximately two weeks before admission and ended officially on day +63.
As I am sure you can tell, there is a large focus on prophylactic and anti-nasea medications initially. The purpose of that is to really try and get ahead of any problems before they begin.
For the first few days, I think it’s really worthwhile to focus on the anti-nausea meds specifically. I recommend asking your care team to walk you through the specific medications being used in your case and the other options they have available, as they often have a deep roster that they can call on depending on the effectiveness of the ones they start you with.
You’ll definitely start to recognize a few of the names as you move through the process, and you’ll find that some work better for you than others. A little trial and error may be necessary at first though.
Before moving on, I want to call out Chlorhexidine (Peridex) specifically. It’s an oral rinse that is used to prevent gingivitis and bacterial infections in the mouth.
If during the first few days of treatment you find yourself thinking, “I could really go for a shot of limoncello right now,” first, you may have a problem the transplant won’t solve. Second, you are in luck, because that is exactly what the chlorhexidine rinse tastes like.
Saying that the first rinse was jarring is an understatement, although it’s pretty amusing in hindsight. Just when you think, “how could this experience get any worse,” they subject you to limoncello shots twice a day.
And no, there aren’t other flavor options. Just have a laugh if you can and get it down.
Transplant & Early Recovery (Day 0 – +17)
Before diving into the medications and treatments I received on or after day 0, I want to take a moment to provide more details about my donor, as I think this is important information to cover. After all, the success of my entire experience, both short- and long-term, almost entirely depends on how well my donor’s cells do what they are supposed to do and how they interact with my body.
Donor Details
In my case, I received an allogeneic transplant using actual marrow product from my donor. Allogeneic essentially means not directly related. Even though nobody else in my family had the GATA2 mutation, my team didn’t want to take any unnecessary risks, so we opted to look outside my immediate family for a match.
She was found on the national registry, which most transplant centers have access to and use to search for potential donors.
My donor was chosen for a few reasons. Most importantly, she was a 10/10 HLA match, in her early thirties, and available. Arguably, those are the three biggest factors right there.
In addition, she had the same blood type as me, which most transplant centers would consider a “secondary consideration”—valuable input but far less important than the main factors listed above.
My donor being female was another factor in their decision. This mismatch can increase what doctors call the graft-versus-leukemia effect (GVL). Because all the cells in my body contain male-specific markers, my new immune system would hopefully be able to recognize any residual blood cells that carried the mutation and other male-specific markers as not belonging.
They are not targeting “male” cells simply because they have those markers, but it does make those cells more easily recognizable to my new immune system. I hope that makes sense.
While that sounds great on paper, it can also increase the risk of graft-versus-host disease (GVHD), since doctors cannot pre-select which cells will be targeted, and just about every cell in my body contains male-specific markers. It was a slight increase in risk that was considered along with all the other factors, but eventually was still deemed the most effective plan of action in my scenario.
As far as I know, those were the key details my team took into consideration when choosing my donor. If you’d like to learn more about the process as a whole, I recommend this article by NMDP, which provides a clear outline of the search process and addresses many other commonly asked questions.
Okay, with that covered, let’s jump back into the actual treatment and medications.
Chemotherapy Agents
Unfortunately, a bit more chemotherapy is usually necessary after receiving the transplant to help ensure that the engraftment process goes as smoothly as possible.
- Cyclophosphamide (Cytoxan) – Cytoxan differs from the two agents already discussed in the fact that I received it after the transplant. It acts as a prophylactic, with the goal of preventing any immediate GVHD from occurring by targeting and destroying T-cells that are active in your body. How it goes about that is above my level of being able to translate, so I am going to once again refer you elsewhere to learn more about the specifics should you be interested.
- My Dosage: 3,400mg in sodium chloride 0.9%. 287 mL. IV infusion. 2 doses total. Administered every 24 hours. Each dose took roughly 2 hours. First dose on day +3. Last dose on day +4.
Additional Medications
Deep breath folks. Here we go again. In this instance, the medications listed below are the ones that I started on or after day 0.
- Amoxicillin (Augmentin) – Used to treat/prevent bacterial infections in multiple different areas of the body, notably the ears, lungs, nose, skin, urinary tract, etc.
- My Dosage: 875mg. Oral medication. Every 12 hours. First dose on day +5. Last dose on day +9. Replaced Levaquin due to skin reaction.
- Aprepitant (Cinvanti) – Used to reduce the severity of chemotherapy induced nausea and vomiting.
- My Dosage: 130mg. IV Injection. First and only dose on day +3. Administered prior to initial Cytoxan dose.
- Calcium Carbonate – An antacid that is commonly used to treat heartburn, acid reflux, indigestion, etc.
- My Dosage: 1,000mg. Oral medication. Every 4 hours as needed. First dose on day +7. Last dose on day +12.
- Cepacol (Lozenge) – Given to aid in reducing mouth and throat discomfort.
- My Dosage: 1 pill. Oral medication. Up to 3 times a day as needed. First dose on day +15. Last dose on day +16.
- Clindamycin (Cleocin T) – An antibiotic that is commonly used to treat acne, or in my case, inflammation of the hair follicles on my legs.
- My Dosage: 1% strength. Topical cream. Once or twice daily as needed. First introduced on day +2. Last used on day +14.
- Dicyclomine (Bentyl) – Typically used to treat patients suffering from irritable bowel syndrome. Can be used in the transplant setting to reduce bowel discomfort.
- My Dosage: 10mg. Oral medication. Up to 3 times a day as needed. First dose on day +9. Last dose on day +12.
- Diphenhydramine (Magic Mouthwash) – Yup, that’s what it’s actually called. Essentially serves as a numbing agent that can reduce the discomfort associated with mucositis.
- My dosage: 15mL. Oral rinse. Up to 4 times a day as needed. First introduced on day +13. Last dose on day +19.
- Diphenoxylate (Lomotil) – Essentially an anti-diarrhetic that works by slowing down intestinal movement.
- My Dosage: 2.5mg. Oral medication. Up to 4 times a day as needed. First dose on day +10. Last dose on day +11.
- Esomeprazole (Nexium) – Typically used to treat certain conditions that result in too much acid being in your stomach.
- My Dosage: 20mg. Oral medication. Once a day as needed. First dose on day +2. Last dose on day +17.
- Famotidine (Pepcid) – Commonly used for stomach ulcers, acid reflux, heartburn, and other similar issues.
- My Dosage: 20mg. Oral medication. Up to 2 times a day as needed. First dose on day +2. Last dose on day +17.
- Filgrastim-Ayow (Releuko) – An injection that is given to patients to help their bone marrow produce white blood cells. Commonly given during the early recovery period to boost counts so patients can be safely discharged.
- My Dosage: 480 mcg. Subcutaneous injection. Once a day. First dose on day +5, continued until ANC count was greater than 500 for 2 consecutive days. Last dose on day +17 prior to discharge.
- Furosemide (Lasix) – Typically used to treat fluid retention and hypertension. In the transplant setting, it is given to increase the amount of urine the body produces.
- My Dosage: 20mg. IV injection. Every 6 hours. First dose on day +3. Last dose on day +5. Taken alongside receiving cytoxan to keep urine output at atleast 200 ml/hr.
- Guaifenesin (Robitussin) – An ingredient typically found in cough and cold medicines that helps to clear mucus.
- My Dosage: 200mg. Liquid solution. Every 8 hours as needed. First dose on day +3. Last dose on day +6.
- Hydroxyzine (Atarax) – An antihistamine commonly used to treat anxiety, itching, hives, etc.
- My Dosage: 25mg. Oral medication. Every 6 hours as needed. First and only dose on day +3.
- Lactated Ringer’s – An odd name for sure. Essentially, this infusion just helps replace water and electrolytes in your system.
- My Dosage: 1,000 mL. IV injection. Administered over 2 hours. First and only dose on day +15.
- My Dosage: 500 mL. IV injection. Administered over 1 1/2 hours. First and only dose on day +16.
- Levofloxacin (Levaquin) – An antibiotic typically used to treat certain types of bacterial infections. Used as a prophylaxis in the transplant setting. Also, fun fact, can also be given to patients who “have been exposed to anthrax or certain types of plague.” Who knew.
- My Dosage: 500mg. Oral medication. Once a day. First dose on day +2. Last dose on day +4.
- Loperamide (Imodium) – An anti-diarrhetic that acts by targeting and slowing down certain receptors in your gut.
- My Dosage: 4mg. Oral medication. Up to 4 times a day as needed. First dose on day +7. Last dose on day +10.
- Loratadine (Claritin) – Just your everyday antihistamine. Used to treat runny nose, sneezing, hives, etc.
- My Dosage: 10mg. Oral medication. Once a day. First dose on day +3. Last dose on day +7.
- Magnesium Citrate – A supplement used to maintain healthy magnesium levels that can also double as a laxative.
- My Dosage: 296mL. Liquid solution. Once a day as needed. First and only dose on day 0.
- Magnesium Oxide (Mag-Ox) – Essentially the same as magnesium citrate. Used to maintain healthy magnesium levels.
- My Dosage: 400mg. Oral medication. Three times per day. First dose on day +16. Last dose on day +70. Stopped after coming off Ursodiol.
- Men-euc-thy-camp-benz-naci-pot (Alkalol) – A mouthwash given to help reduce mucus and soothe discomfort in the mouth.
- My Dosage: 15mL. Oral rinse. Every 6 hours. First dose on day +4. Last dose on day +15.
- Mesna (Mesnex) – Typically given to lower the risk of inflammation and bleeding in the bladder to patients receiving certain chemotherapies.
- My Dosage: 680mg in sodium chloride 0.9%. IV infusion. Once a day. First dose on day +3. Last dose on day +4. Administered before receiving Cytoxan.
- My Dosage: 680mg in sodium chloride 0.9%. IV infusion. Three times a day. First dose on day +3. Last dose on day +4. Administered after receiving Cytoxan.
- Mycophenolate Mofetil (Cellcept) – An immunosuppressant that is given to help suppress your immune system to allow your transplant to settle.
- My Dosage: 1,000mg. Oral medication. Three times a day. First dose on day +5. Last dose on day +28.
- Oxybutynin (Ditropan) – A medication typically given to help reduce the frequency of spasms in the bladder and urinary tract.
- My Dosage: 5mg. Oral medication. Up to 3 times a day as needed. First dose on day +6. Last dose on day +8.
- Oxycodone – A painkiller offered to patients during the transplant process to reduce more severe discomfort.
- My Dosage: 2.5-5mg. Oral medication. Every 4 hours as needed. DID NOT TAKE.
- Phenazopyridine (Pyridium) – A medication typically given to reduce pain or discomfort in the urinary tract.
- My Dosage: 200mg. Oral medication. Three times a day. First dose on day +5. Last dose on day +12.
- Phytonadione (Vitamin K1) – A vitamin supplement of sorts given to combat vitamin K deficiency and to treat bleeding or blood-clotting disorders caused by other medications/treatment.
- My Dosage: 10mg. Oral medication. First and only dose on day +13.
- Potassium Chloride (KCL) – Used to treat or prevent low levels of potassium in the blood. Potassium is crucial to many essential bodily functions.
- My Dosage: 20 mEq/50 mL. IV infusion. Every hour as needed, depending on potassium level. Started regular dosing on day +7. Ended on day +17.
- Pramoxine – A topical lotion typically used to treat pain, itching, dryness, etc.
- My Dosage: 1%. Topical cream. Up to 3 times a day as needed. First and only application on day +1.
- Senna (Senokot) – Used to relieve mild constipation.
- My Dosage: 2 tablets. Oral medication. 2 times per day as needed. Taken on day 0 and day +1.
- Simethicone (Mylicon) – Given to reduce excess pressure in the stomach and intestines caused by gas.
- My Dosage: 80mg. Oral medication. Every 6 hours as needed. First dose on day +9. Last dose on day +13.
- Sodium Chloride – Administered to maintain healthy fluid and electrolyte levels.
- My Dosage: 0.9% bolus. 1,000 mL. IV infusion. First dose on day +12. Last dose on day +13.
- My Dosage: 0.9% bolus. 500 mL. IV infusion. First dose on day +3. Last dose on day +4. Alongside receiving cytoxan to keep urine output steady.
- Tacrolimus (Prograf) – An immunosuppressive agent that is meant to prevent your body from rejecting the transplant.
- My Dosage: 0.5mg. Oral medication. Twice a day. Dosage depending on prescribed intake. First dose on day +5. Last dose on day +139.
- My Dosage: 1mg. Oral medication. Twice a day. Dosage depending on prescribed intake. First dose on day +5. Last dose on day +139.
A lot of these medications, similar to those in the conditioning section, are prophylactic, meaning they are meant to prevent issues from occurring rather than treat the issues they are commonly used for.
That said, where the list starts to differ is that many of these attempted to address specific problems that began to appear as my time in the hospital continued.
Oxybutynin and Phenazopyridine, for example, were given in response to the hemorrhagic cystitis I developed shortly after finishing my doses of Cytoxan. Magnesium Citrate was given when I had trouble producing bowel movements, and Senna was prescribed when that issue very quickly ended up on the other end of the spectrum.
You get the point. A good chunk of the medications you end up taking at this point in the process will largely be in direct response to your specific needs.
The one medication I want to highlight specifically is Tacrolimus, my immunosuppressant. You will likely start your specific immunosuppressive agent shortly after receiving the transplant and continue taking it until your team decides to start tapering you off, often many months later.
Needless to say, it’s an important one. It is one of the main tools that your team will prescribe you that will attempt to ensure that your transplant actually has time to settle and hopefully prevent any immediate and drastic immune reactions from occurring.
Most immunosuppressants come with side effects so it is absolutely worth having a basic understanding of your team’s drug of choice so you can be aware of what to keep an eye out for and what your team will be monitoring for as you continue to take it.
Post-Transplant (Day +18 – Present Day)
Discharge, while absolutely something to celebrate, does not mean you are done taking medications. Before being let out, you will meet with your care team and a pharmacist who will walk you through what medications you will need to take once you are no longer in the hospital.
It will not be a short list.
While it can feel overwhelming at first, like everything else related to the transplant experience, you would be surprised at what you and your caregivers are able to get somewhat used to.
What follows below is a list of all the medications I have been prescribed since discharge. You may recognize most of them, as I started many while still in the hospital.
The list is broken down into short-term medications, those I stopped within a few months of discharge, and long-term medications that I am still currently taking roughly eight months post-transplant.
Short-Term
- Atovaquone – Prescribed to prevent the growth of a certain fungus that typically leads to pneumonia.
- My Dosage: 5mL. Liquid solution. Once a day. First dose on day +18. Last dose on day +28.
- Magnesium Oxide (Mag-Ox) – Essentially the same as magnesium citrate. Used to maintain healthy magnesium levels.
- My Dosage: 400mg. Oral medication. Three times per day. First dose on day +16. Last dose on day +70. Stopped after coming off Ursodiol.
- Mycophenolate Mofetil (Cellcept) – An immunosuppressant that is given to help suppress your immune system to allow your transplant to settle.
- My Dosage: 1,000mg. Oral medication. Three times a day. First dose on day +5. Last dose on day +28.
- Tacrolimus (Prograf) – An immunosuppressive agent that is meant to prevent your body from rejecting the transplant.
- My Dosage: 0.5mg. Oral medication. Twice a day. Dosage depending on prescribed intake. First dose on day +5. Last dose on day +139.
- Ursodiol (Actigall) – Actigall works as a prophylactic, with the goal of preventing any liver issues as treatment begins and during recovery.
- My Dosage: 300mg. Oral medication. Three times a day. Began approximately two weeks before admission and ended officially on day +63.
Long-Term
- Acyclovir (Zovirax) – Traditionally used to treat shingles, herpes (HSV), and chickenpox. Used in the transplant setting as an anti-viral/prophylaxis to prevent these from occurring or resurfacing while your new immune system re-builds.
- My Dosage: 400mg. Oral medication. Three times a day. First dose on day -5. Have taken daily since.
- Cholecalciferol (Vitamin D3) – Dietary supplement used to treat vitamin D deficiency. In addition to supporting your bone health, having a healthy vitamin D level actually supports your immune system as well, which is crucial in the early stages of recovery.
- My Dosage: 25mcg. Oral medication. Once a day. First dose on day -1. Have taken daily since.
- Folic Acid (Folvite) – Supports your body’s ability to produce healthy and functional red blood cells.
- My Dosage: 1mg. Oral medication. Once a day. First dose on day -5. Have taken daily since.
- Multivitamin (MVI) – Provides your body with nutrients you may or may not be receiving enough of through your diet.
- My Dosage: 1 pill. Oral medication. Once a day. First dose on day -5. Have taken daily since.
- Sulfamethoxazole-Trimethoprim (Bactrim) – A medication typically given to treat or prevent certain types of infections. Replaced Atovaquone as my main infection/pneumonia deterrent once my platelet count had recovered enough.
- My Dosage: 160mg. Oral medication. Once a day. First dose on day +28. Have taken daily since.
In terms of calling out any specific one of these medications, I don’t have much to really add. They are all important, and after discharge, it’s more about getting used to being responsible for administering your own medications every day than anything else.
It’s setting alarms, making sure your caregivers know what you need to be taking, keeping track of supply, and so on. Logistical things, really.
That said, I would be remiss if I did not mention just how truly disgusting Atovaquone is. It is a neon yellow liquid, not unlike what you might get if you melted down a yellow highlighter, and taking a small swig of that every day for the first week and a half after discharge was pretty unpleasant.
I was eventually switched to a different anti-pneumonia medication, but that only happened once certain cell counts had recovered enough.
There are many factors your team will consider before prescribing medications post-transplant, and how a medication affects your counts is just one of them. As a result, you may end up taking some version of a nasty yellow highlighter juice for a week or two should your team deem it necessary.
Side Effects & Management
Now that we have covered all the medications and such, I want to take some time to talk about the specific side effects and issues I developed during my time in the hospital. I will save discussing my current issues, none of which are all that concerning, for my periodic Field Note updates.
We’ll be going through these one at a time in the exact order they appeared.
Just as a reminder, these are not universal, they are simply the issues that I personally experienced.
Folliculitis
- Folliculitis – A common skin issue that is caused by hair follicle inflammation or infection. Symptoms began on day +2.
Compared to the other three issues I will be covering, this one was very minor. It is exactly what it sounds like, just inflammation of certain hair follicles.
As you can see from the photo below, this mainly affected the shin area on both of my legs. It was not painful, just noticeable.
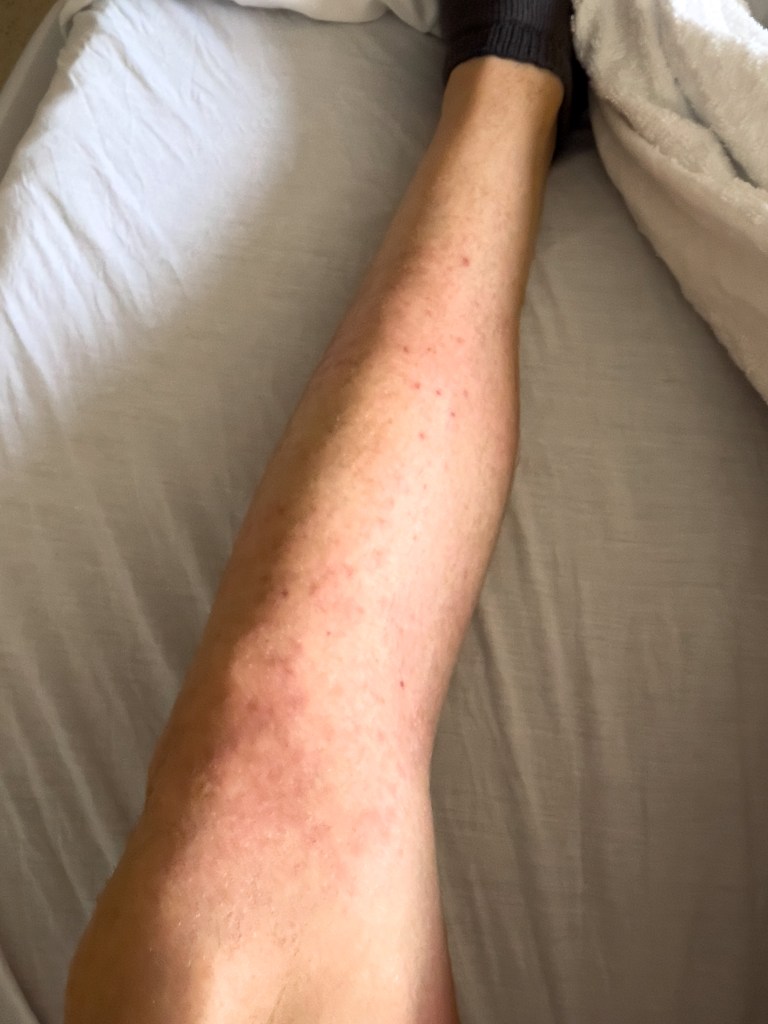
This quickly took a backseat, as it was around the same time that I started developing the next issue, which we are about to discuss.
Erythema
- Erythema – A skin reaction typically caused by an infection or in response to a certain medication. Symptoms began on day + 3.
Pictured below are two photos of the erythema I experienced. The one on the left was taken on day +3, and the one on the right on day +7. The reaction started below the knees on both sides and extended up to my abdomen, lower back, and along the sides of my chest.
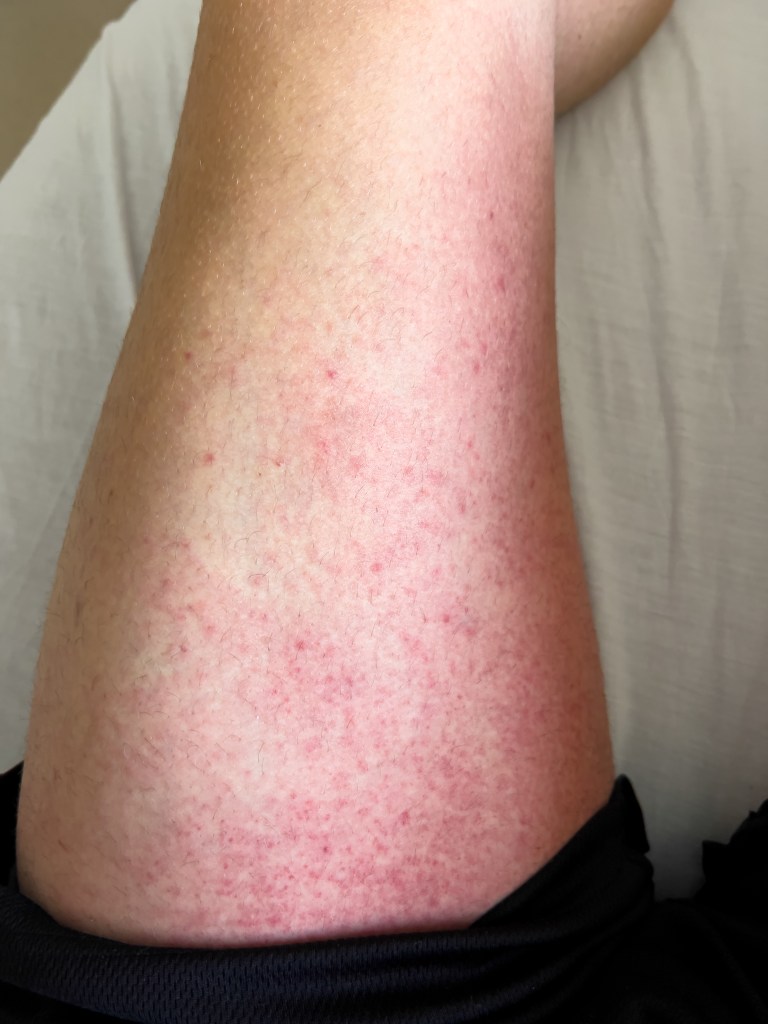
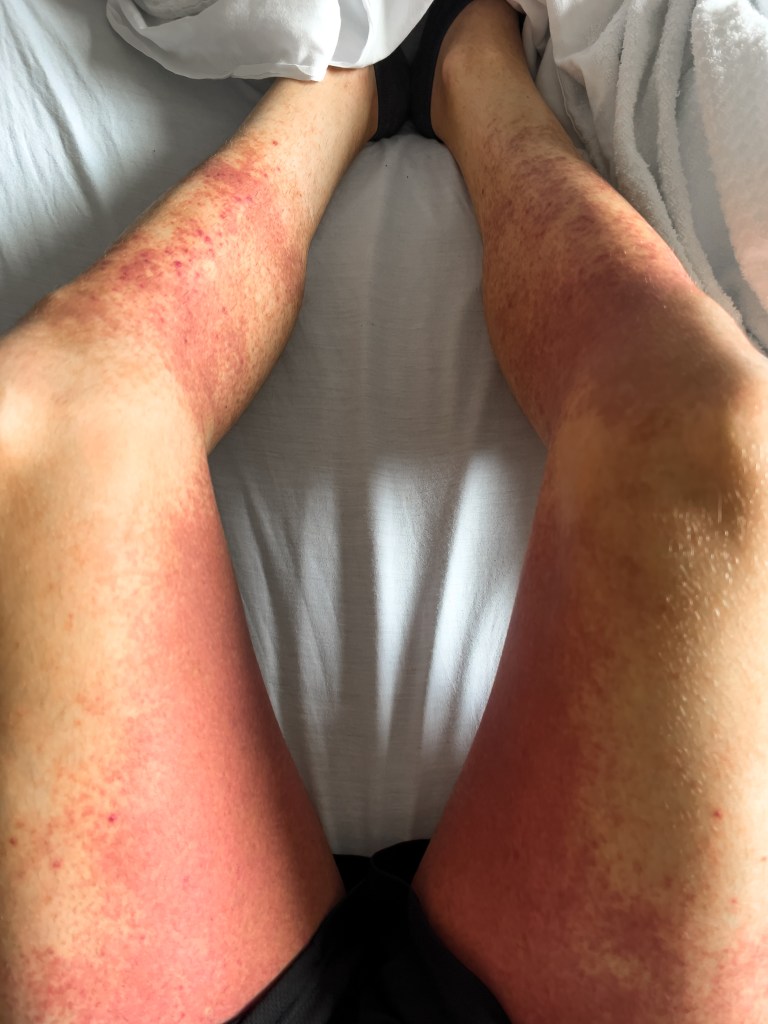
While it certainly looks painful, I would be lying if I said I experienced any itching or pain in the affected areas. It was alarming to look at and to watch it spread at first, but it was more cosmetic than anything else.
To this day, I am not entirely sure if this reaction was caused by one of the chemotherapy agents or by the Levaquin I took. My records point to Levaquin, but I think both explanations are plausible.
My skin did heal, but it took time. For a week or two, the affected areas were the bright red you see in the second photo. It was not until after I was discharged that the color began to fade to a duller brown, and it took a few months before the skin in those areas looked normal again.
Hemorrhagic Cystitis
- Hemorrhagic Cystitis – A medical condition that occurs when the lining of your bladder becomes inflamed and bleeds. Symptoms began on day + 5.
The cystitis was probably the most uncomfortable direct side effect I experienced from treatment, and it ended up being the one that persisted the longest.
The lining of your bladder is fragile even on a good day, and unfortunately, the Cytoxan I received is known to occasionally cause damage in that area.
When the issue first appeared and as it continued, my team emphasized the importance of staying hydrated to keep things moving through my system. While that made sense, in practice it meant going to the bathroom more often, which only served to increase the discomfort.
The issue gradually improved the further I got from transplant, but it took a solid three to four months before blood stopped occasionally appearing in my urine, and a little longer than that for the discomfort to meaningfully subside. Even eight months out, I still notice the occasional discomfort.
Mucositis
- Mucositis – Inflammation of the mucosa, which is essentially part of the lining of your GI tract that goes from your mouth all the way through your intestines. Symptoms began on day +13.
A close second for the most uncomfortable issue that I experienced. I was lucky in that my mucositis wasn’t too severe, and I was still able to eat on my own, but it was very uncomfortable and not something I looked forward to enduring each day.
There are certain mouthwashes and medications that can help while dealing with mucositis, but the truth is they only do so much.
This issue eventually began to heal as my white cell count increased and my new immune system gradually worked to repair the mouth sores, though it did take some time.
Misc.
You may have noticed that the short list did not include chemo-induced nausea and vomiting, loss of appetite, diarrhea, headaches, weight loss, brain fog, and so on. I didn’t think those needed much elaboration, as they are fairly self-explanatory and are definitely more common with this type of treatment.
I experienced all of them at differing levels of severity.
While not fun to deal with, I was more prepared to experience them and they required less active management than the ones I specifically called out above.
Lessons Learned & Tips
This section could easily be its own post, but I don’t think that would be too helpful to anyone quite frankly. Everyone’s experience will be unique, so I’m going to keep it high level and just focus on one thing I wish I had prepared for or understood better before admission.
While receiving chemotherapy is certainly a challenging part of this process, I would argue that it’s what comes afterwards that deserves more attention.
The best way to describe it is like a three-punch combo. Your counts start to drop, side effects start to appear, and mentally the days start to drag on and become more taxing.
Before that happens, there is a lot going on, and while it is absolutely overwhelming, there is structure.
Once the transplant has been received though, the structure fades a little bit. While you will certainly still be taking mandatory medications and receiving planned treatment, your care becomes more reactive in a lot of ways.
It turns into a waiting game that is not very fun to participate in.
It’s arguably when you will need to lean on those around you the most and have the most faith in your care team and the treatment itself.
Unfortunately, nobody can take the discomfort of those days away. I can’t promise they won’t be hard. They absolutely will. But I can tell you from firsthand experience that those days do eventually end, even when it feels like they never will.
You’ll quickly learn that “one day at a time” goes from a slightly overused platitude to the only way to get through.
Closing Thoughts.
And there we have it, a more or less complete overview of my transplant.
The goal of this post was not to overwhelm but to inform. To provide a real-life example of what receiving a stem cell transplant could look like.
If you are preparing for your own transplant and came across this post during your research, I want to say one last thing. While the experience will absolutely be challenging, you will be in the hands of some of the most caring and experienced healthcare professionals in the world.
They will be there for you every single step of the way.
One of the first things I was told on my first night in the hospital was that the goal of transplant is not to make you suffer. Your team will consider every discomfort you experience and work to make it more manageable. They will have backups in place and be prepared for nearly every curveball this treatment can throw.
Take comfort in that. Trust your care team, trust your support crew, and trust yourself to get through this.
Talk soon,
Ethan
Resources
Misc. links directly referenced in this article:
- Veno-Occlusive Disease (VOD)
https://cancer.ca/en/treatments/side-effects/veno-occlusive-disease - Sinusoidal Obstruction Syndrome (SOS)
https://www.merckmanuals.com/professional/hepatic-and-biliary-disorders/vascular-disorders-of-the-liver/sinusoidal-obstruction-syndrome - Alkylating Agent
https://www.britannica.com/science/alkylating-agent - Myeloablative Chemotherapy
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/myeloablative-chemotherapy - Types of Stem Cell Transplants
https://www.dana-farber.org/health-library/types-of-stem-cell-transplant - Allogeneic Stem Cell Transplant
https://www.mayoclinic.org/tests-procedures/allogeneic-stem-cell-transplant/pyc-20384863 - HLA Typing
https://www.nmdp.org/patients/understanding-transplant/finding-a-donor/hla-typing-matching - Graft-Versus-Leukemia Effect (GVL)
https://www.yalemedicine.org/clinical-keywords/graft-versus-leukemia-effect - Graft-Versus-Host Disease (GVHD)
https://my.clevelandclinic.org/health/diseases/10255-graft-vs-host-disease-an-overview-in-bone-marrow-transplant - National Marrow Donor Program (NMDP)
https://www.nmdp.org/patients/understanding-transplant/finding-a-donor - Deep Vein Thrombosis (DVT)
https://www.mayoclinic.org/diseases-conditions/deep-vein-thrombosis/symptoms-causes/syc-20352557
Chemotherapy Agents:
- Busulfan – Busulfex
https://www.mayoclinic.org/drugs-supplements/busulfan-intravenous-route/description/drg-20067303- Research Paper: https://pmc.ncbi.nlm.nih.gov/articles/PMC4261695/#S4
- Cyclophosphamide – Cytoxan
https://www.mayoclinic.org/drugs-supplements/cyclophosphamide-oral-route-intravenous-route/description/drg-20063307 - Fludarabine – Fludara
https://www.mayoclinic.org/drugs-supplements/fludarabine-intravenous-route/description/drg-20063840- Research Paper: https://pmc.ncbi.nlm.nih.gov/articles/PMC4812520/
Additional Medications:
- Acyclovir – Zovirax
https://www.mayoclinic.org/drugs-supplements/acyclovir-oral-route-intravenous-route/description/drg-20068393 - Amoxicillin – Augmentin
https://www.mayoclinic.org/drugs-supplements/amoxicillin-oral-route/description/drg-20075356 - Aprepitant – Cinvanti
https://www.webmd.com/drugs/aprepitant-emend - Atovaquone
https://www.webmd.com/drugs/atovaquone - Bisacodyl – Dulcolax
https://www.webmd.com/drugs/bisacodyl - Calcium Carbonate
https://my.clevelandclinic.org/health/drugs/20402-calcium-carbonate-chewable-tablets - Cepacol – Lozenge
https://www.drugs.com/cdi/cepacol-sore-throat-benzocaine-menthol-lozenges.html - Chlorhexidine – Peridex
https://www.mayoclinic.org/drugs-supplements/chlorhexidine-oral-route/description/drg-20068551 - Chlorhexidine Gluconate
https://www.mskcc.org/cancer-care/patient-education/how-bathe-using-2-chg-cloths - Cholecalciferol – Vitamin D3
https://www.mayoclinic.org/drugs-supplements/cholecalciferol-oral-route/description/drg-20088484 - Clindamycin – Cleocin T
https://www.mayoclinic.org/drugs-supplements/clindamycin-topical-route/description/drg-20063064 - D-5-½ NS with KCL 20
https://www.drugs.com/pro/potassium-chloride-in-dextrose-and-sodium-chloride.html - Dicyclomine – Bentyl
https://www.drugs.com/mtm/dicyclomine.html - Diphenhydramine – Magic Mouthwash
https://www.medicalnewstoday.com/articles/magic-mouthwash#what-it-is
Mucositis: https://my.clevelandclinic.org/health/diseases/24181-mucositis - Diphenoxylate – Lomotil
https://www.mayoclinic.org/drugs-supplements/diphenoxylate-and-atropine-oral-route/description/drg-20061751 - Enoxaparin – Lovenox
https://www.mayoclinic.org/drugs-supplements/enoxaparin-intravenous-route-subcutaneous-route-injection-route/description/drg-20063670
DVT: https://www.mayoclinic.org/diseases-conditions/deep-vein-thrombosis/symptoms-causes/syc-20352557 - Esomeprazole – Nexium
https://www.mayoclinic.org/drugs-supplements/esomeprazole-oral-route/description/drg-20074322 - Famotidine – Pepcid
https://www.mayoclinic.org/drugs-supplements/famotidine-oral-route/description/drg-20072972 - Filgrastim-Ayow – Releuko
https://www.mayoclinic.org/drugs-supplements/filgrastim-ayow-intravenous-route-subcutaneous-route/description/drg-20530920 - Folic Acid – Folvite
https://www.mayoclinic.org/drugs-supplements-folate/art-20364625 - Furosemide – Lasix
https://www.drugs.com/furosemide.html - Guaifenesin – Robitussin
https://www.drugs.com/guaifenesin.html - Hydroxyzine – Atarax
https://www.drugs.com/hydroxyzine.html - Lactated Ringer’s
https://www.mayoclinic.org/drugs-supplements/lactated-ringer-s-intravenous-route/description/drg-20489612 - Lactulose – Constulose
https://www.mayoclinic.org/drugs-supplements/lactulose-oral-route/description/drg-20528356 - Levetiracetam – Keppra
https://www.mayoclinic.org/drugs-supplements/levetiracetam-oral-route/description/drg-20068010 - Levofloxacin – Levaquin
https://www.drugs.com/levofloxacin.html - Loperamide – Imodium
https://www.drugs.com/loperamide.html - Loratadine – Claritin
https://www.drugs.com/loratadine.html - Lorazepam – Ativan
https://www.mayoclinic.org/drugs-supplements/lorazepam-oral-route/description/drg-20072296 - Magnesium Citrate
https://www.drugs.com/mtm/magnesium-citrate.html - Magnesium Oxide – Mag-Ox
https://www.drugs.com/mtm/magnesium-oxide.html - Magnesium Sulfate
https://www.mayoclinic.org/drugs-supplements/magnesium-sulfate-oral-route-topical-application-route-route-not-applicable/description/drg-20088513 - Men-euc-thy-camp-benz-naci-pot – Alkalol
https://healthfully.com/28003-use-alkalol.html - Mesna – Mesnex
https://www.mayoclinic.org/drugs-supplements/mesna-oral-route/description/drg-20095304 - Multivitamin – MVI
https://www.webmd.com/vitamins/ai/ingredientmono-1400/multivitamins - Mycophenolate Mofetil – Cellcept
https://www.drugs.com/mtm/mycophenolate-mofetil-oral-injection.html - Neomycin – Neo-Fradin
https://www.drugs.com/mtm/neomycin.html - Olanzapine – Zyprexa Zydis
https://www.drugs.com/olanzapine.html - Ondansetron – Zofran
https://www.mayoclinic.org/drugs-supplements/ondansetron-oral-route-oromucosal-route/description/drg-20074421 - Oxybutynin – Ditropan
https://www.drugs.com/oxybutynin.html - Oxycodone
https://www.drugs.com/oxycodone.html - Palonosetron
https://www.mayoclinic.org/drugs-supplements/palonosetron-intravenous-route/description/drg-20065261 - Phenazopyridine – Pyridium
https://www.drugs.com/mtm/phenazopyridine.html - Phytonadione – Vitamin K1
https://www.drugs.com/mtm/phytonadione-oral-injection.html - Polyethylene Glycol
https://www.drugs.com/mtm/polyethylene-glycol-3350.html - Polymyxin B
https://www.drugs.com/cdi/polymyxin-b.html - Potassium Chloride – KCL
https://www.drugs.com/potassium_chloride.html - Pramoxine
https://www.drugs.com/mtm/pramoxine-topical.html - Prochlorperazine – Compazine
https://www.mayoclinic.org/drugs-supplements/prochlorperazine-oral-route/description/drg-20406263 - Senna – Senokot
https://www.mayoclinic.org/drugs-supplements/senna-oral-route/description/drg-20406012 - Simethicone – Mylicon
https://www.drugs.com/mtm/simethicone.html - Sodium Chloride
https://www.medicinenet.com/sodium_chloride_solution-intravenous/article.htm - Sulfamethoxazole-Trimethoprim – Bactrim
https://www.mayoclinic.org/drugs-supplements/sulfamethoxazole-and-trimethoprim-oral-route/description/drg-20071899 - Tacrolimus – Prograf
https://www.mayoclinic.org/drugs-supplements/tacrolimus-oral-route/description/drg-20068314 - Ursodiol – Actigall
https://www.mayoclinic.org/drugs-supplements/ursodiol-oral-route/description/drg-20066618
Issues/Side Effects
- Erythema
https://my.clevelandclinic.org/health/diseases/24475-erythema-multiforme - Folliculitis
https://my.clevelandclinic.org/health/diseases/17692-folliculitis - Hemorrhagic Cystitis
https://my.clevelandclinic.org/health/diseases/24164-hemorrhagic-cystitis - Mucositis
https://my.clevelandclinic.org/health/diseases/24181-mucositis
Leave a comment